Macular degeneration, a commonly occurring eye ailment, has the potential to greatly affect an individual’s eyesight and overall quality of existence. It is a condition that often creeps into the lives of older adults, leading to a gradual loss of central vision. Dealing with macular degeneration can be difficult, but gaining a comprehensive understanding of this ailment is essential for its successful control. Macular degeneration is not a monolithic disease; rather, it comes in two primary forms: wet and dry. In this article, we’ll delve into the difference between wet and dry macular degeneration, their treatment options, and ultimately, which is the more challenging adversary.
What is Macular Degeneration?
Before diving into the specifics of wet and dry macular degeneration, let’s establish a foundational understanding of the condition itself. Macular degeneration, commonly known as age-related macular degeneration (AMD), is a gradual eye condition that predominantly impacts the elderly population. It stands as one of the leading causes of irreversible vision loss among this demographic, posing a significant threat to their visual health and overall well-being.
Essentially, macular degeneration focuses on the macula, a tiny yet crucial section of the retina responsible for central vision. The macula enables us to perceive fine details, colors, and the sharpness of objects. When macular degeneration strikes, it compromises the macula’s integrity, leading to a blurred or distorted central vision.
Now that we’ve established the essence of macular degeneration, let’s delve deeper into the contrasting realms of wet and dry macular degeneration.
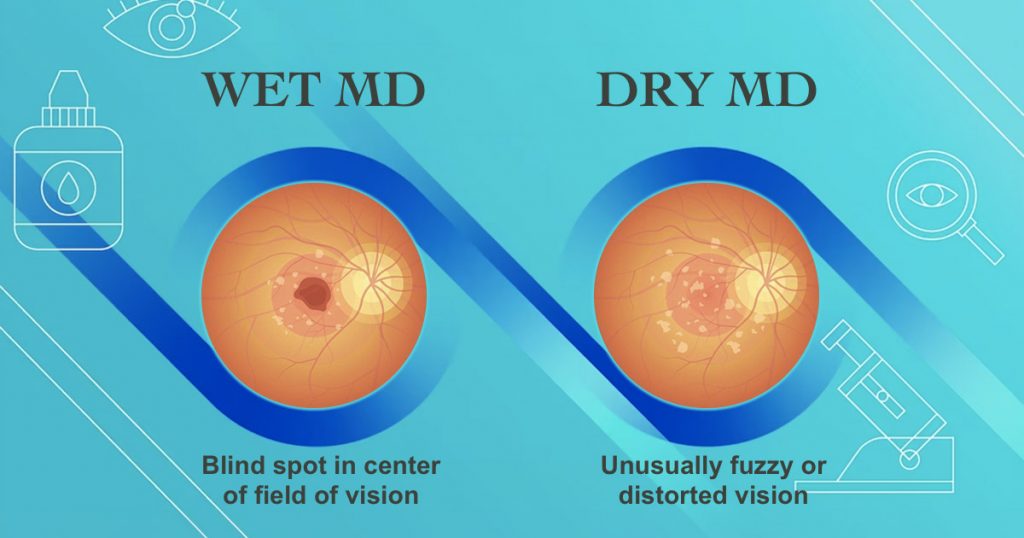
Wet Vs Dry Macular Degeneration – What’s the Difference?
One of the key distinctions in the world of macular degeneration lies in its classification into two primary types: dry and wet. The main difference between these two types lies in their underlying mechanisms and the severity of vision impairment they can inflict.
Dry Macular Degeneration

This form of macular degeneration, also known as non-neovascular AMD, constitutes the majority of cases, encompassing roughly 80% of those diagnosed with AMD. Dry AMD manifests when the light-sensitive cells in the macula gradually deteriorate over time. A defining characteristic of dry AMD is the presence of drusen, clusters comprised of lipids and proteins, beneath the macula. These drusen, while not necessarily causing immediate vision loss, serve as markers of potential trouble down the road.
Symptoms of dry AMD often develop subtly, if they’re noticed at all, making early diagnosis critical. These symptoms may include:
- Dark spots or smudges in vision, particularly noticeable in the morning
- Faded colors
- Increased sensitivity to bright lights
- Perception of straight lines as bent or wavy
- Challenges in reading, with words seemingly disappearing
- Difficulty adapting to changes in lighting
Wet Macular Degeneration

In contrast, wet macular degeneration, also referred to as neovascular AMD, represents a smaller percentage of AMD cases but packs a more severe punch. This form of AMD is characterized by the growth of abnormal blood vessels beneath the retina, which can lead to fluid leakage and damage to the surrounding tissues. The buildup of fluid and blood in the retinal region can lead to notable distortions in one’s vision.
The unique aspect of wet macular degeneration is that it typically begins as dry AMD, with the gradual breakdown of the macula. However, dry AMD does not always progress to the wet form. It’s important to note that the term “dry” does not imply a lack of discomfort; rather, it signifies the absence of wet AMD’s particular characteristics.
Symptoms of wet AMD can be more abrupt and may include:
- Straight lines appear bent or distorted.
- Blurry central vision or blind spots within the visual field.
- Difficulty adjusting to varying light conditions.
- Impaired ability to discern fine details without ample lighting.
- Challenges in recognizing faces.
Which is Worse: Dry or Wet Macular Degeneration?
Now that we’ve explored the unique characteristics of both dry and wet macular degeneration, it’s natural to ponder which of these adversaries is more formidable. In this context, severity is a critical factor to consider.
- Wet Macular Degeneration – Certainly, wet macular degeneration is the more serious of the two conditions. The rapid onset of symptoms, distortion in vision, and the potential for significant fluid leakage all contribute to the increased seriousness of wet AMD. Left untreated, it can lead to substantial vision loss and impairment of daily activities.
- Dry Macular Degeneration – While dry AMD is more common and progresses gradually, it is generally less severe than its wet counterpart. Numerous people with dry AMD encounter slight vision impairment along with the existence of large, soft drusen in the retina. However, dry AMD can worsen over time, potentially resulting in central vision loss if left unmonitored or untreated.
An essential aspect to consider is that dry AMD can transition to wet AMD, albeit less commonly. Regular monitoring by an eye specialist is crucial for early detection and intervention, particularly in individuals with dry AMD.
How Do You Treat Macular Degeneration?
The treatment landscape for macular degeneration varies between dry and wet forms.
- Dry Macular Degeneration – Presently, dry AMD lacks a definitive cure, but there are ongoing clinical trials investigating potential therapeutic options. Promising breakthroughs include stem cell therapies, Apl-2 injections, the oral antibiotic Oracea, and the anti-inflammatory drug Metformin. While these treatments are in various phases of research, they may not be widely available for several more years.
- Wet Macular Degeneration – Treatment for wet AMD has advanced more significantly. The primary approach involves the use of anti-VEGF medications, which inhibit the protein responsible for the growth and leakage of blood vessels in the eye. These drugs are delivered through injections into the vitreous cavity located at the rear of the eye. While effective, they may require repeated treatments every few weeks to months.
Both Macular Degeneration are Bad, But Wet AMD is Worse
In the realm of macular degeneration, understanding the difference between wet and dry forms is essential for patients and their caregivers. While both types can result in blurriness, visual changes, and challenges in daily life, wet AMD stands out as the more severe and rapidly progressing variant. Early diagnosis, regular eye exams, and adherence to lifestyle factors that reduce AMD risk are key elements in managing both forms of this condition.
With ongoing research delving into innovative treatment options, there is optimism for enhanced results and a more promising future for individuals dealing with macular degeneration. Whether dry or wet, early intervention and vigilance remain the best allies in the battle against this vision-threatening adversary.