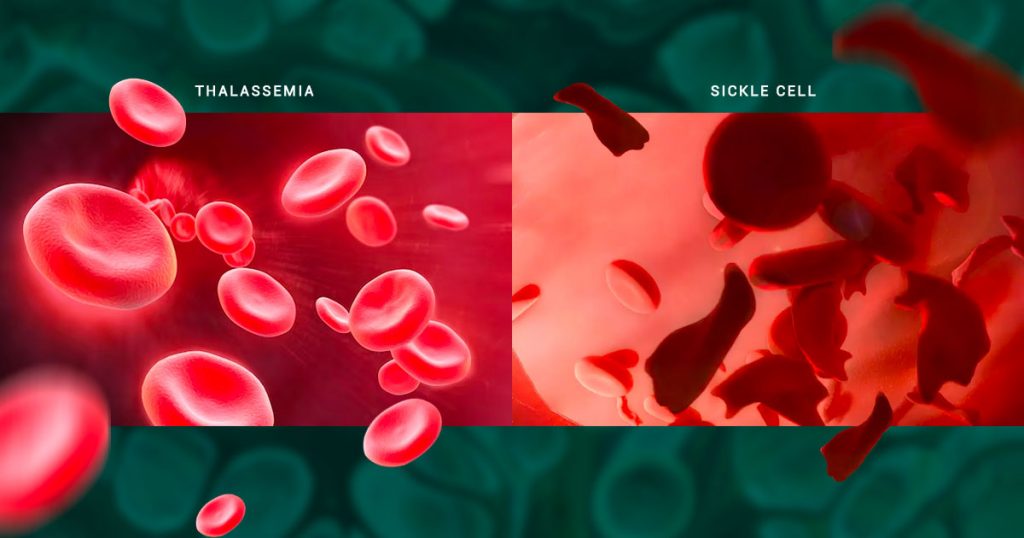
Genetic conditions such as sickle cell disease and thalassemia interfere with the body’s ability to produce hemoglobin, a protein found in red blood cells that transports oxygen throughout the body. Although both conditions can lead to anemia and other serious health problems, they are caused by different genetic mutations and have different impacts on the body.
These disorders are not uncommon. A study showed that thalassemia had a prevalence rate of 3.96%, whereas sickle cell anemia had a prevalence of 1.98%. In daily life, these diseases can lead to fatigue, weakness, and in severe cases, can even interfere with normal activities due to pain or complications.
The diagnosis of these disorders is crucial as it allows healthcare professionals to implement appropriate treatment strategies. This guide will help elucidate the differences between Thalassemia and Sickle Cell disease.
Thalassemia: Definition, Prevalence, and Symptoms
Thalassemia is a group of inherited blood disorders marked by low hemoglobin production. It is classified as alpha or beta thalassemia depending on which part of the hemoglobin is affected. The severity of thalassemia varies according to the specific type and number of mutations.
The prevalence of β-thalassemia was reported to be 2.12%. Thalassemia symptoms include fatigue, weakness, pale or yellowish skin, facial bone deformities, slow growth, abdominal swelling, and dark urine. The effects on the body can be significant, leading to issues like iron overload, bone deformities, and cardiovascular illness.
Sickle Cell Disease: Definition, Prevalence, and Symptoms
Sickle cell disease is a severe hereditary form of anemia in which a mutated form of hemoglobin distorts red blood cells into a crescent shape when oxygen levels are low. It is most prevalent in people of African descent. Sickle cell trait was found to be present in 1.81% of people.
Symptoms of sickle cell disease typically appear in childhood. They include anemia, recurrent infections, and periodic episodes of pain known as crises. The complications of sickle cell disease can affect nearly every organ system in the body, leading to conditions like stroke, acute chest syndrome, blindness, bone damage, and ulcers.
Knowledge of Sickle Cell Disease and Thalassemia Severity
Determining which condition, thalassemia or sickle cell disease, is more dangerous is a complex process that hinges on various factors. These include the specific type of disorder, severity of symptoms, and an individual’s overall health status.
Type of Disorder
Thalassemia and sickle cell disease have different types that can influence severity. Thalassemia, for instance, is classified into alpha or beta types, depending on which part of hemoglobin is affected. The alpha type usually leads to less severe symptoms, while the beta type can cause serious health problems.
Similar to this, there are various types of sickle cell disease, including sickle cell trait and sickle cell anemia. People with sickle cell trait generally have no symptoms, while those with sickle cell anemia experience severe symptoms and complications.
Severity of Symptoms
The severity of symptoms also plays a crucial role in determining the danger level of these conditions. Sickle cell crises, characterized by episodes of severe pain, can be debilitating and may require hospitalization. In contrast, people with thalassemia may experience varying symptoms, ranging from mild anemia to severe complications requiring regular blood transfusions.
Individual Health Status
An individual’s overall health status is another important factor. Those with strong immune systems and good overall health may cope better with these conditions, while those with other underlying health issues may face more severe complications.
Despite the potential severity of both conditions, it’s crucial to remember that with appropriate treatment and management, many individuals with these conditions can lead full and active lives. There have been significant improvements in medical therapies that frequently effectively prevent or manage complications.
For instance, painkillers, blood transfusions, and occasionally a bone marrow transplant can all be used to treat sickle cell crises. The same goes for those who have thalassemia, who may need blood transfusions, iron chelation therapy to get rid of extra iron, and in extreme cases, a stem cell transplant.
Early Signs and Recommendations
Early signs of sickle cell disease typically appear in childhood and include anemia, infections, and periodic episodes of pain. The body can experience pain episodes anywhere, while anemia can lead to exhaustion, pallor, and shortness of breath. The frequency and duration of these episodes can vary greatly between individuals.
Early indications of thalassemia can include weakness, weakness, pale or yellow skin, deformities of the facial bones, slow growth, abdominal swelling, and dark urine. Depending on the type of thalassemia, these symptoms can range greatly in severity.
You should seek medical attention right away if you or your child displays any of these symptoms so they can be evaluated. Blood tests and genetic testing can confirm a diagnosis of these disorders. Effective management of these conditions and the avoidance of complications depend on early detection.
Mitigating Symptoms of Thalassemia and Sickle Cell Disease
While thalassemia and sickle cell disease can both lead to serious health issues, there are a number of methods and treatments that can be used to control symptoms and enhance quality of life.
Thalassemia
The type and severity of the disease determine the course of treatment for thalassemia. Here are some ways to mitigate its symptoms:
Blood transfusions
For those with severe thalassemia, regular blood transfusions are a common form of treatment. This helps replenish the body’s red blood cell count and normal hemoglobin levels.
Iron chelation therapy
This treatment is often necessary for individuals receiving regular blood transfusions, as these can lead to an iron overload in the body. Iron chelation therapy uses medication to help remove the excess iron.
Folic acid supplements
These can help the body produce more red blood cells.
Bone marrow or stem cell transplant
For severe cases, a bone marrow or stem cell transplant from a compatible donor can potentially cure thalassemia.
Sickle Cell Disease
Managing sickle cell disease involves preventing crises, treating symptoms, and avoiding complications. Here are some strategies:
Pain-relieving medications
Over-the-counter pain relievers and prescription medications are commonly used to alleviate the pain during a sickle cell crisis.
Hydroxyurea
This prescription medication can lessen the frequency of acute chest syndrome and pain crises. It may also decrease the need for blood transfusions.
Blood transfusions
Regular blood transfusions can lower a child’s risk of stroke and help adults with sickle cell disease avoid complications.
Bone marrow transplant
This is currently the only potential cure for sickle cell disease, but it’s not an option for everyone due to the significant risks involved and difficulty finding suitable donors.
Routine vaccinations and preventive antibiotics
These are essential for managing sickle cell disease because it can increase an individual’s susceptibility to infections.
In addition to these therapies, upholding a healthy lifestyle can aid in controlling both conditions’ symptoms. This entails maintaining a healthy weight, working out frequently, getting enough rest, and avoiding stress and extreme weather as triggers.
Sickle Cell Disease and Thalassemia: Treatment Options and Support
Throughout our exploration of thalassemia and sickle cell disease, we’ve seen that while they share similarities as inherited blood disorders, they present unique challenges in terms of their causes, symptoms, and treatment approaches. To effectively manage these conditions and enhance the quality of life for those who are affected, it is essential to comprehend these differences.
However, beyond medical treatments and therapies, the role of support from doctors, families, and loved ones cannot be overstated. Regular interaction with healthcare professionals is vital not only for monitoring the disease and adapting treatment plans, but also for gaining access to resources and services, such as genetic counseling and patient advocacy groups.
Family support is equally essential. The journey with thalassemia or sickle cell disease can be challenging, and having a strong support network can provide emotional comfort, practical help, and the encouragement to adhere to treatment regimens.
In conclusion, living with thalassemia or sickle cell disease requires a comprehensive approach that combines medical interventions with robust emotional and social support systems. With this in place, those who suffer from these conditions can still lead happy, fulfilling lives.